My Blog
Western Medicine
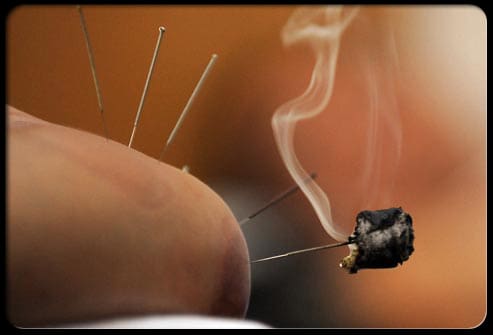
Acupuncture and Western Medicine
Let’s Take A Stab At It!
By Jill Ellen Smith L.A., M.Ac.
For the Howard County Women’s Journal
A patient recently suggested I write an article helping people to understand how one could combine the use of acupuncture and western medical treatments. A lot of people think it’s an either/or… an oppositional conversation.
As an RN, professionally born and bred at both the University of Maryland and Johns Hopkins Hospitals, I completely embraced the Western medical model. It made sense to me and it worked –a lot of the time. It was clearly linear in its approach. A patient had symptoms…a diagnosis was made which usually fell in one or two categories, and treatments that had already been tested and proven statistically significant were prescribed. A patient recovered or improved; or minimally responded, or didn’t respond at all. A patient went home… or died. There was comfort in the relative predictability of it all.
As an acupuncturist I learned to dwell in the world of grays and muted tones—not an easy transition from the black and white more definitive hallowed halls of Johns Hopkins. Chinese medicine’s diagnostic process followed a fairly well-defined approach as well, while simultaneously being very fluid and expansive. In the search for a source of the symptoms, a practitioner will illuminate an underlying pattern of disharmony that will often involve multiple organ and bodily systems. The precision and intricacy of Eastern medicine was hidden much deeper within the diagnostic process.
So what does all this mean to the consumer who wants to balance the benefits of both cultural approaches? It means that the possibilities are grand!
Consider the patient who breaks a bone and goes to the ER to have it set. An acupuncturist’s needle is not capable of setting a bone. However, what if this bone doesn’t heal well or a chronic pain condition develops from it? This is where, along with analgesics and possibly antibiotics, acupuncture can make a huge difference. The acupuncturist is trained to determine what is preventing proper healing or what is creating the chronic pain. An acupuncturist will determine the source of the problem. And, ideally over time the analgesics will become lessened or terminated; the antibiotics will become unnecessary.
And what of the patients who do not respond to Western approaches or improve only minimally? These patients are optimum candidates for acupuncture. Acupuncture can enhance the treatments that are already being instituted by an MD. For example, a diabetic may find that the insulin is managed at a lower dose. Or a patient with ulcerative colitis may have less flare ups or use less medication. Most frequently, patients learn to live with their disease or disability maximally so that it no longer consumes their life. In other word, they learn to manage the disability rather than have their condition manage them.
Recently, I developed an acute urinary tract infection several days after a routine colonoscopy. Although I knew from a Chinese medical perspective that I had ‘heat in my lower Jiao’ it was my MD I wanted—and quickly. Once it was under control, I was able to deal with the underlying issue related to the source of my problem with my acupuncturist. She dealt with the underlying pattern of disharmony with a focus on preventing any further infections.
Recently a patient prone to nosebleed’s had a major one. While we recognized the issue of ‘heat in his upper Jiao’ (Chinese medicine divides the body into 3 sections or Jiao), that couldn’t be dealt with until he had the nasal blood vessel cauterised by his doctor. His MD dealt with managing the symptom while, we continue a treatment approach to work on the source of his nosebleed’s. The heat in his system determines what action is used on the needle and which points are selected, as well as lifestyle alterations he needed to make.
Many women request non-Western approaches to menopausal symptoms from their gynecologist. Acupuncture and possibly herbs are methods of therapy that can tailor themselves to these issues.
A patient with glaucoma finds that his pressure in his eye decreased to within normal limits after a series of treatments with his acupuncturist. He was ultimately able to decrease his medication for that condition.
A patient of mine with a history of a serious post-partum depression nearly nine years ago is preparing to taper down and possibly stop taking her antidepressant. She got through this past Fall/Winter season with ease while in acupuncture treatment and now is eager to try life without her antidepressant. She is preparing to wean herself off while under the supervision of her psychiatrist. She will increase her acupuncture treatments to weekly while we follow through with our treatment plan. For the first time “in my life” (as she will declare) she is not afraid.
Chinese medicine is the quintessential preventive medicine practice. Because the acupuncture diagnostic process goes to the source of our dis-harmonies and imbalances, the very nature of the treatments become preventative. By attaining optimum balance in one’s body through regular acupuncture treatments, any preexisting medical condition abates or becomes more responsive to Western treatments. From cancer (where acupuncture is particularly effective in treating the treatment side effects), to sleep disorders that have not responded to anything but addicting drugs — acupuncture can supplement and complement Western medical approaches.
There is nothing oppositional about East and West. Like Yin and Yang.
Testimonial
As a dancer I have had years of back pain, and more recently insomnia associated with menopause. For the first time I have found substantial and consistent relief from both. Jill’s gentle and caring guidance has led me to a new awareness of my body. Her expertise has truly been invaluable.
Lucy H. – Baltimore, MD
